The global pandemic has led to some tectonic changes in the realm of healthcare. Please describe them.
Satya Nadella, the CEO of Microsoft, recently said that the digital transformation of healthcare has led to more change in the last six months than, could have been expected over the next six years. And he’s right. Since this all started last March, KPMG teams have been working on more than 95 engagements globally, focusing on everything from regional test capacity to PPE supply chains to creating patient engagement apps. As a result of this work, I have identified 10 key characteristics of the new world of healthcare that is unfolding around us [see below].
The first characteristic is perhaps the most significant: The new ‘digital front door’. At the high point of the first wave last March and April, 80 to 85 per cent of medical consultations in developed nations were taking place either virtually or telephonically. In January of 2020, the average percentage for these countries was less than two per cent. So, we have witnessed an enormously accelerated digital revolution.
By 2030, there will be a global shortfall
of 18 million healthcare workers.
Your latest book focuses on another, less-recognized healthcare crisis. Please describe it.
Put simply, there is too much work to be done and far too few workers. The World Health Organization estimates that by 2030, there will be a shortfall of 18 million healthcare workers, which represents 20 per cent of the total capacity of care — a shortage of one in five required workers. I do believe we can close this shortfall through a combination of factors, which I discuss in detail in my book. These include embracing digital technology and artificial intelligence; encouraging individuals to take responsibility for their own health; and encouraging governments to be more entrepreneurial, including enacting more progressive immigration legislation.
Some of the solutions are quite simple, like extending the retirement age for workers. The Netherlands’ Advisory Committee on Medical Manpower Planning worked out that if the doctors who wanted to postpone retirement and work two years longer were able to do so, its total supply of doctors would grow by four per cent between 2006 and 2030 instead of falling by one per cent.
Education also plays a role, as there are many more students trying to enter the caring professions than there are places in university programs. The UK’s National Health Service currently employs about 26 per cent of its doctors from abroad (often from poorer countries that cannot afford the brain drain) while large numbers of domestic applications to get trained are turned down. In 2018, there were close to 21,000 applicants for just over 6,500 places. Given the coming shortfall, this simply must change.
10 Characteristics of Healthcare’s New Reality
|
|
Digital front-door: The only front door. Hospital outpatient and general practitioner appointments across the world have been transformed with as much as three-quarters of all consultations now taking place virtually.
‘Clean’ and ‘dirty’ sites (Green and Blue). In response to the pandemic, health systems across the globe have introduced strict infection control measures including the separation of COVID and non-COVID patients, to prevent spread in hospitals and care homes.
‘Hot ’ and ‘cold’ sites: New patient flows. Cold sites deliver non-COVID care in order to lower infection risk , operate efficiently without interrupting acute work and create capacity for elective procedures. Establishing hot and cold sites will be imperative to delivering the kind of new patient flows necessitated by COVID-19. Public Private Partnerships have been formed in some countries to help expand public sector capacity in this way.
Scaled-up primary care and centralized specialty services. With COVID-19, we have seen a continued push by health systems towards delivering care in the right setting, especially in out-of-hospital care settings (e.g. primary care, home and community care, etc.). This rapid increase in demand has exposed the lack of scale and centralization of the primary care and specialty services, which will be necessary in facilitating any health system’s entry into the post-COVID-19 new reality.
Aged care services: Achilles heel? Managing the spread of the virus has been a challenge in long-term care facilities across the globe.
Supply-chain resilience and back-office scale. The coronavirus has exposed the vulnerabilities of offshore and ‘just in time’ supply chains that rely on lean manufacturing principles. Greater resilience can be achieved through larger inventories; supplier diversification; and nationalization or regionalization of supply chains.
Command centres. Realizing the importance of data-driven insights in strategic and operational decision making, some countries have set up command centres similar to air traffic control systems to manage c are more efficiently.
Agile workforce. To prepare for a ‘staff slump’ due to physical, mental and emotional exhaustion and support operations in a post-COVID-19 new reality, workforce models will need to transform to become agile, employ data-driven insights, and empower their workers.
Institutional and health-system governance. COVID-19 has exposed the need to work collaboratively to deal with the challenges it has placed on the workforce, supply chains and infrastructure.
Project management: The need for speed. Given the fast-paced nature of the changes being implemented in most health systems, an agile project management approach has been adopted by some countries. For instance, in the UK the NHS employed this approach when it converted an exhibition centre into a temporary hospital in just nine days.
|
Will the shortfall be similar across countries?
No, it will be highest among upper middle-income countries, driven by growing economies, populations and aging. And these shortages will fuel global competition for skilled health workers at just the time that nationalism is gaining traction. Middle-income countries will face shortages too, as demand exceeds supply. But low-income countries will face low growth in both demand and supply, and will not likely be able to meet the United Nations Sustainable Development Goals for health and well-being, which set ambitious targets for disease reduction and health equity (including universal health coverage by 2030). Every country signed up to the development goals, but they now need to spell out how they will play their part in delivering universal health coverage, ensuring they make their fair contribution to the pool of global health talent.
Can you touch on the role of technology in addressing this crisis-within-a-crisis?
It has been estimated that 36 per cent of all healthcare tasks can be supported by machine learning, robotics or artificial intelligence. The challenge will be figuring out which tasks can be supported by which technology. In our work, my team and I have a process where we look at ‘care pathways’.
We basically map out all the various stages of the patient experience, clarify in detail the care processes and administrative tasks involved in each, and then we look at how each step can supported or supplemented with technology. That’s one way to get started on this.
You have said that “Unless we have activated patients, no system in the world can be sustainable.” Please explain.
We all need to take personal responsibility for our health. In developed countries, we now know that long-term chronic diseases like heart disease and diabetes drive 70 per cent of healthcare costs. We also know these diseases can be either reversed, stopped, or maintained at a decent level through patient behaviour. That is why ‘activating’ patients as partners in their own care is so critical.
We know from our research that there are four levels of patient activation, with level one being the lowest and level four being a highly activated patient. At level four, the clinician serves more like a coach. Studies indicate that these patients’ use between eight and 21 per cent less healthcare. It makes sense for everyone involved. I have worked in parts of Africa, which carries 25 per cent of the world’s disease burden (yet has only four per cent of the world’s healthcare workforce). In such cases, patient activation is literally a matter of life and death.
How to Tackle the Health Workforce Crisis
|
|
1. Reframe and reposition the debate about work-force planning to one about productivity, health and national wealth creation.
2. Encourage governments to become more entrepreneurial, stimulating health worker supply through a host of measures ranging from the relaxation of training limits to increased labour participation rates for healthcare.
3. Encourage the rapid and large-scale adoption of new models of care that already exist in different parts of the world so that enhanced well-being, prevention, promotion, care and treatment can increase productivity and capacity to care.
4. Provide the human and technological support to enable patients to be active partners in their care, taking greater responsibility for their own well-being and the management of long-term conditions.
5. Provide greater recognition, encouragement and support for communities, volunteers and families, who already provide most of the care in society.
6. Support health professionals to practice at the upper limits of their clinical license, encouraged by regulators.
7. Create a new cadre of care assistants and workers who seamlessly straddle health and social care to deliver services in communities, hospitals and homes.
8. Stimulate the disruptive digital possibilities offered by artificial intelligence, cognitive assistance, robotics and blockchain to increase time to care and productivity.
9. Embrace digital technology to create agile learning systems that educate, re-educate and support workers.
10. Overhaul rudimentary approaches to the leadership development and coaching of individuals and teams, embracing proven techniques that raise motivation and performance.
|
How would you define value-based healthcare? And how is it progressing?
At its simplest, value-based healthcare is ‘the outcome divided by the quality and cost’. Every country in the world wants higher quality care and less cost. There have been experiments in the U.S. and New Zealand where they’ve tried to implement value-based care lock, stock, and barrel — but it’s easier said than done. Many countries choose instead to take steps towards value-based care, by adopting ‘integrated care’ or ‘accountable care’ programs.
To implement true value-based care, you need to track patient pathways very closely so you can unify primary, tertiary, community and home-based care, and you need longitudinal studies on patient well-being and outcomes. No system in the world is there yet. In Canada, the fee-for-service model in your hospitals can make value-based care very difficult to achieve. But it also makes it even more important to talk about it.
On that note, it was once believed that Canada’s healthcare system was a model for the world. How would you summarize our current situation?
Canada faces some significant challenges. You have a wonderful universal health system. You only need to look south of the border to appreciate what you’ve got. You also have some wonderful world class research and magnificent global education. But that said, as you know from various Commonwealth Fund surveys, Canada now ranks number 10 out of the 11 countries they measure. Your costs are far too high, your waiting lists are way too long, and your outcomes are average. So at the moment, Canada is not getting a high grade, and I believe it’s because you have separated primary care from secondary care, and you have a fee-for-service model. With an aging population, you’ve also got a huge volume of people with long-term conditions that need to be managed outside of hospital, either at home or in the community, or by expanding primary care. In countries like the UK, we have a capitation-based formula which allows for better population health management. There are provinces that have started to experiment, notably Ontario (especially Toronto), so I’m hopeful that Canada will improve its position. But for a long time, it has been too complacent.
Given what we’ve all been through over the past year, are we going to be ready when the next crisis hits? Or will we be lucky, and this will never happen again?
People say that these pandemics come along once every century, and it is true that the last one was the Spanish Flu of 1918. The answer to your question is twofold. First, no country will ever leave its emergency planning to chance again. The cost to human and economic life has simply been intolerable. I believe that leaders will want to make sure they have a well-oiled and well thought-through contingency plan at a national, regional and local level. I do not believe that any country will ever again be so unprepared.
Second, we can be hopeful about the future of humanity. Some of these vaccines were created in 10 months, when they would normally have taken 10 years. I truly hope I don’t see another pandemic in my lifetime, but either way, I have the utmost faith in scientists and humanity. If there is one thing to celebrate at this awful time, it is that human beings and Scientific progress have brought solutions to the world in record time.
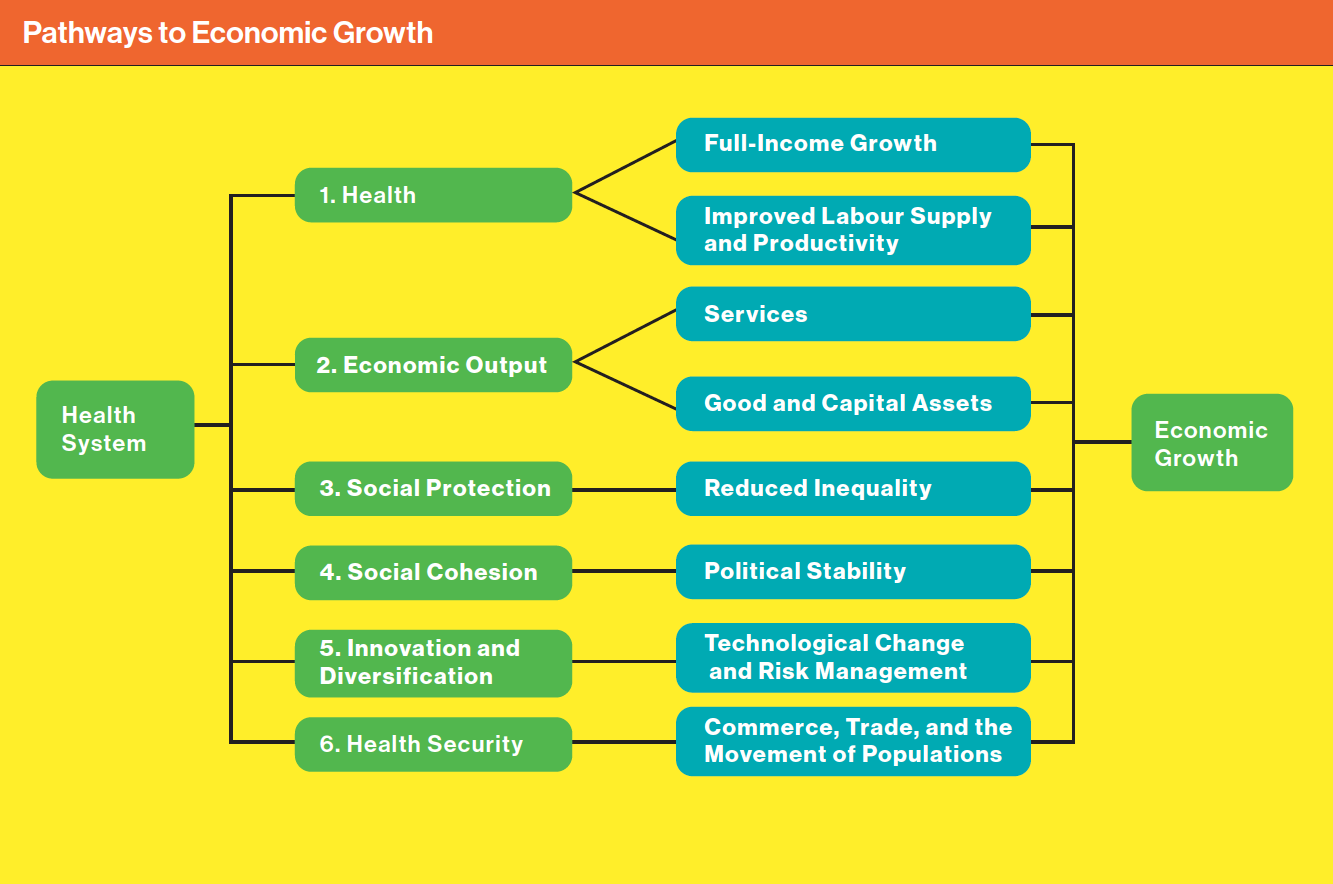
Going forward in our fractured world, health has an enormous role to play in building hope and social cohesion, and a well-trained, technologically productive workforce is good for families, society and economies. With concerted effort, by 2030 we can supply sufficient healthcare staff, reimagine service delivery, harness technology, extend healthy life expectancy and increase the economic well-being of nations. And we must — because if anyone ever doubted it, surely the events of the past year have made it clear that health is wealth.

Mark Britnell is the Global Head of Healthcare, Government & Infrastructure at KPMG International and a member of the World Economic Forum’s Health Council. In January 2021, he joined the Rotman School of Management as an Executive-in-Residence. In this role, he will work closely with the School’s Sandra Rotman Centre for Health Sector Strategy.
Share this article: